What Is a Slipped Disc Really?
Many patients arrive at our clinic having been told they have a “slipped disc,” but the term itself is often misused and can be misleading. Discs don’t actually slip; instead, they bulge, which means the disc is pushing out of its normal space. They may also herniate, which is when the outer layer of the disc tears, allowing the inner gel-like material to push through. In more severe cases, the disc material can protrude or extrude, pushing it even further out and sometimes pressing on nearby nerves. Each stage reflects a different degree of disc disruption and potential nerve involvement.
As a chiropractor in Surbiton who focuses on disc problems, we spend a lot of time helping patients understand that language like “slipped” can underestimate how complex these injuries really are and why they need more than a quick crack to fix.
We use accurate diagnostic language because words influence how people perceive their condition.[2] “Slipped” sounds easily reversed, i.e. with a quick crack; however, we know that “compressed” or “herniated” discs require far more care and planning to resolve. A proper prognosis can only be delivered with an accurate diagnosis, setting the tone for realistic expectations and an effective approach.[2][3]
Clinic director’s personal note: one of the most challenging periods in my life was when I herniated my own disc following a fall hiking. It led to the foundation of The DISC Chiropractors in Surbiton, due to the necessity to understand and successfully treat myself. One step along the journey took me to an eye-opening Facebook page on Disc Injuries and sciatica, where it was sad to read the hostility towards chiropractors who had performed overzealous adjustments on active herniations, resulting in flare-ups in pain. It’s only fair to mention that some patients had the opposite miraculous improvements… the likely deciding factor being the level of damage the patient already had, correctly estimated by the clinician in question.
How Slipped Discs Affect Movement and Nerve Function
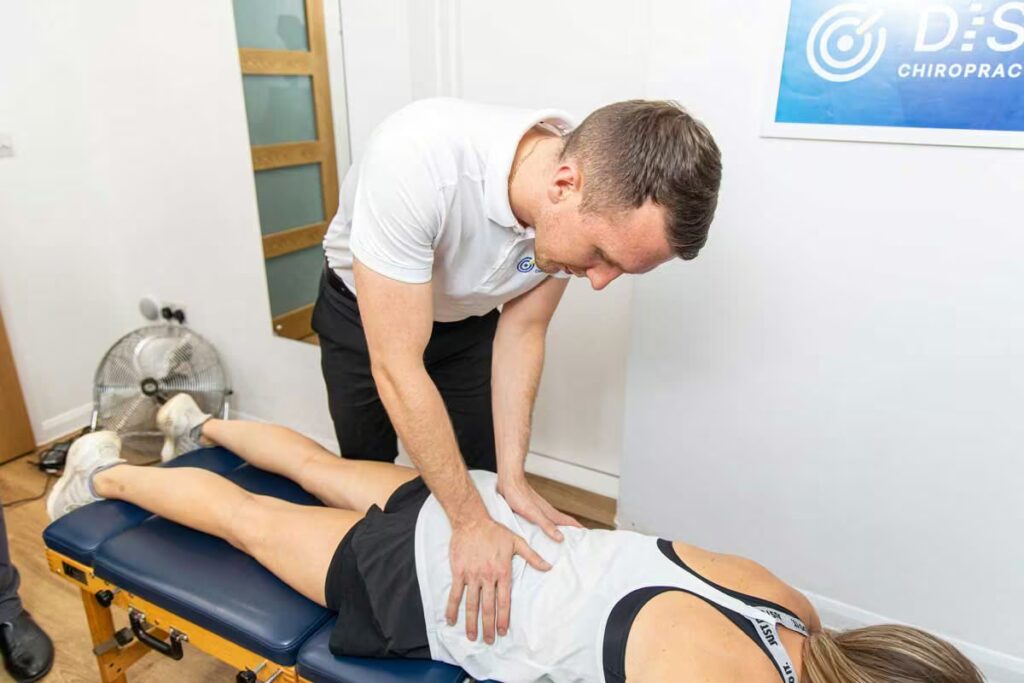
Slipped or herniated discs often affect more than just the spine; they disrupt movement, posture, and muscle control in visible, predictable ways.[1][2] One of the most common presentations we see is a patient arriving in an antalgic posture: leaning or twisted away from the painful side, hips shifted to compensate, and often unable to stand fully upright. This is a pattern our team at The DISC Chiropractors in Surbiton sees every week in people who have “just bent down” and suddenly cannot stand up straight.
Recognising these symptoms can help you understand the impact your condition may have and motivate you to seek effective treatment.
Other classic signs include:
• A semi-flexed or bent knee on the affected side to reduce nerve tension
• Difficulty flexing forward (tying shoes, picking items off the floor)
• Reduced or painful spinal extension (standing tall, arching backwards)
• Resting/seated discomfort and frequent repositioning
These compensations may appear dramatic, but they are often the body’s way of unloading the disc and avoiding further nerve irritation. It’s crucial to recognise these postural adaptations as intelligent responses, highlighting the body’s cleverness in protecting itself from harm. Left unaddressed, these compensatory strategies can lead to further joint dysfunction, nerve damage, and muscle wasting.[1]
We assess not only what hurts, but how the body moves, or avoids moving, as a result.[2] By recognising these functional deficits early, your local Surbiton Chiropractor can tailor treatment to calm the irritated disc while rebuilding proper mechanics.
It’s also important to distinguish between mechanical compression (where the disc physically presses on a nerve root) and chemical irritation (inflammatory by-products affecting nearby nerve tissue).[1][2] Both contribute to symptoms, and both must be accounted for in the treatment strategy.
Why Most Treatments Fail (And What We Do Differently)
Many patients come to us after months, or even years, of bouncing between treatments that offered temporary relief but failed to deliver true, lasting recovery. Shockingly, 50% of chronic back pain sufferers still report pain after 6 months of generic care, with some studies placing the number as high as 89% after one year. These treatments often include generalised physiotherapy or exercise prescriptions that ignore disc-healing timelines. [Donald Murphy](Crawford et al., 1994)
They might also involve prolonged rest and painkillers that mask symptoms but do not correct mechanics, or overly aggressive spinal manipulation that flares up inflammation or nerve sensitivity.[2][3][5][7] However, patients who have followed our DISC Injury Protocol report significant improvement: 80% experience relief and restored function, offering a compelling reason for optimism and a new lease on life.
Contrast this with our DISC Injury Protocol, where precision and timing determine every step. For instance:
– Instead of general physiotherapy, we employ targeted functional rehab to address specific deficits and core activation.
In place of standard exercises that might pressure a sensitive disc, our approach includes controlled decompression and Class IV laser therapy to reduce disc pressure and calm inflammation.
– Rather than relying on painkillers, we focus on long-term solutions, like high-intensity electromagnetic therapy, to restore and maintain stability.
– We avoid the risks of overly aggressive manipulation by using gentle, strategic interventions to prevent flares.
Each phase is adapted to your body’s needs, ensuring true recovery rather than temporary relief.
The best chiropractors in Surbiton understand that a disc injury is not just another episode of simple backache; it needs specific care… the right plan at the right time, rather than a generic “three sets of ten” sheet.
What these approaches miss is the nuanced progression of disc healing. A herniated or bulging disc is highly reactive in its early phase. It doesn’t respond well to pressure, torsion, or random exercise. More importantly, nerve sensitivity can delay a patient’s tolerance to movement, even as the disc improves.[2][3]
Our approach is built around precision and timing. We:
• Prioritise controlled decompression to reduce disc pressure and restore space around the sacrum roots [8-11]
• Desensitise the nervous system using Class IV laser therapy, light instrument-assisted adjustments, and strategic unloading techniques[5][12-15]
• Layer in progressive rehab only when the disc is stable enough to handle it, avoiding setbacks.
• Continuously reassess and adapt care based on real functional progress, not guesswork.[2][3]
Disc injuries don’t necessarily need more treatments; they need the right treatment at the right stage. That’s the core of our protocol: a clear, research-led roadmap designed to support actual disc regeneration, not just temporary pain relief.[1][8-11] Every phase of our care plan is based on evidence-backed timing and technique, ensuring the right intervention at the right moment. This is the kind of structured approach people often expect from the best chiropractors in Surbiton, rather than an open-ended series of unconnected visits.[2][3][6]
Our audited outcomes confirm that 80% of patients experience at least 80% improvement within the recommended protocol window, a result we attribute to the knowledge, experience, precision, structure, and adaptability of our approach.
The 3-Phase DISC Injury Protocol
Our 9-week program (comprising 18 sessions) is divided into three clearly defined phases: Move, Stabilise, and Fortify. This structured progression reflects the healing trajectory of disc injuries, particularly in cases presenting with altered movement, compensatory posture, or severe neural sensitivity. Once basic movements have been relearned, you’ll move from stabilising your current condition to rebuilding your body’s mechanics, and finally fortifying your resilience against future issues. For many people searching for the best chiropractor in Surbiton after trying other options, this clear, phase-based roadmap is often the missing piece.
Each phase is tailored not only to reduce symptoms but also to progressively correct the dysfunctions that initially cause pain, with the goal of returning the patient to pain-free, independent movement patterns without fear of flare-ups or reinjury.
Phase 1: Stabilise and Calm (Treatments 1–6)
Goals:
• Reduce inflammation
• Decompress the disc and “untrap” the nerve.
• Regain safe foundational movement patterns
Tools:
• Spinal decompression therapy (introduced incrementally based on nerve tolerance and pain reactivity) [8-11]
• Class IV laser therapy (tissue healing and inflammation control) [12-16]
• Instrument-assisted adjusting (gentle, controlled mobilisations) [5]
In severe cases, we may require a pre-treatment triage phase that begins with conservative methods to assess the body’s sensitivity and reactivity. Some patients respond positively to decompression right away, but for others, particularly those with intense inflammation or nerve involvement, a more cautious, defensive approach is required.[2][3] In these situations, Class IV laser therapy is used first to calm irritation and “firefight” inflammation, creating a safer window to introduce decompression progressively. [12-15]
Decompression is not delivered in isolation. It is paired with strategic mechanical interventions such as spinal muscle release, pelvic realignment, and hip mobility corrections. These treatments not only help relax hypertonic musculature but also reduce biomechanical loading on the injured disc. [1-3] This dual-action approach addresses both the functional imbalances that likely contributed to the injury and the heightened reactivity that often blocks early treatment success.
By laying this foundation, we can introduce decompression earlier and more effectively, accelerating care progression without compromising safety or comfort. When someone comes to a Surbiton Chiropractor barely able to stand upright, this calmer stabilisation phase is often the difference between flaring them up and helping them turn the corner.[2][3][8-11]
Phase 2: Rebuild and Retrain (Treatments 7–12)
This is where we go beyond symptom management and begin rebuilding the architecture of movement & stability. At this stage, patients are often upright, more mobile, and eager to resume normal activity, yet beneath the surface, neurological inhibition, scar tissue, and compensation patterns may still persist.[1-3]
We use targeted functional testing to identify asymmetries in load distribution and core activation that persist and inhibit movement. For example, single-leg stance testing, dynamic gait assessments, and segmental strength screens reveal deficits that were previously masked by pain.[2][3]
If untreated, these deficits can reintroduce shear forces to the healing disc or overload adjacent joints. That’s why we address not only what moves, but how it moves. Our aim is to create a movement system that is not just pain-free, but durable, responsive, and capable of adapting to life’s demands without recurring breakdown.[2][3]
Goals:
• Restore proper joint mechanics and global movement
• Correct muscle imbalances and faulty loading patterns
• Reactivate underperforming muscle groups and stabilisers
Tools:
• Functional rehab tailored to patient-specific deficits, including core reactivation drills
• High-intensity electromagnetic therapy (HIEMT) for deep core and pelvic floor stability
• Neuromuscular stimulation (NMS) to restore proper firing patterns in overly sensitive nerve endings or restore nerve-compromised muscle groups
• Radial shockwave therapy to address stubborn scar tissue and chronic soft tissue restrictions[17-20]
• Manual adhesion release to improve mobility, tissue glide, and segmental stability
This phase also gives us the opportunity to build on foundational improvements and adapt to any elements of care that may be lagging. While the protocol provides a clear roadmap, it is not rigid. If a patient shows uneven progress, whether due to prolonged neural inhibition, stubborn movement restrictions, or unpredictable flare-ups, we pivot quickly.
Our clinicians have contingency protocols (Plans B, C, and D) prepared, including targeted therapies, modified rehabilitation progressions, and strategic pauses or resets if Plan A hasn’t fulfilled all our expectations. This flexibility ensures that progress continues, even if it doesn’t follow a straight line.
For patients who have already seen more than one chiropractor in Surbiton or London and still feel fragile, this is often the first time they experience a plan that actually rebuilds capacity instead of stopping at pain relief.
Phase 3: Future-Proof and Fortify (Treatments 13–18)
Goals:
• Build lasting resilience and adaptive movement strategies
• Return confidently to work, activity, or sport without protective hesitation
• Phase out reliance on care through habit-building, education, and self-assessment
Tools:
• Continued decompression (if indicated by load response or remaining symptoms)[8-11]
• Load tolerance drills to reintroduce strength and dynamic movement under real-world forces
• Advanced movement re-education to challenge balance, coordination, and postural endurance
• Lifestyle-specific mobility/stability protocols that integrate with the patient’s unique environment, whether occupational, athletic, or home-based. [2][3]
In this phase, we shift from controlled rehabilitation to real-world resilience, progressing from basic postural stability to dynamic strength and confident movement. It’s not enough for the spine to be supported while lying down or sitting still; the true test is whether it remains stable under load, during unexpected movement, and over extended periods. We aim to challenge and build not just endurance, but responsiveness, so that the spine and surrounding musculature can perform, adapt, and recover automatically, without conscious guarding or restriction. Patients are challenged through progressively more complex tasks and reintroduced to previously provocative positions, such as lifting, twisting, prolonged sitting, or high-impact activities, to confirm stability under stress.[2][3]
To further reinforce self-efficacy during this phase, we encourage patients to track a simple home metric, such as rating their mobility after their warm-up exercise on a scale of 1-10. This empowers them to monitor their progress, validates our phased tapering approach, and strengthens their independence.
We also space out treatment visits to monitor independence. This deliberate reduction in frequency acts as a test: can the patient sustain improvements without continuous input? Are the right postural, ergonomic, and self-management habits in place? Importantly, this final active care phase is where long-term confidence is built. Our aim is not lifetime dependency, it’s lifetime function. We equip patients with the knowledge, exercises, and awareness needed to self-regulate and intervene early if future flare-ups occur. That’s what truly future-proofs recovery. It is the kind of finish people hope for when they seek the best chiropractors in Surbiton, rather than a quick, short-lived fix.[2][3]
The Role of Imaging and Assessment
We use imaging thoughtfully and only when it adds meaningful value to the clinical picture: [1-4] (Diagnostic Imaging Practice Guidelines for Musculoskeletal Complaints in Adults, 2025)
• X-rays are used to rule out structural abnormalities, assess spinal alignment patterns, and establish a baseline view of bone health and degeneration. In cases of suspected nerve involvement (radiculopathy), X-rays are typically performed before initiating care, in accordance with chiropractic regulatory guidance for informed clinical decision-making.
If you believe you may have a disc injury and your chiropractor has not performed or recommended imaging, this could be a clinical red flag worth questioning before continuing treatment. At our clinic, we are committed to ensuring your safety and peace of mind. We carefully assess each patient’s condition and recommend imaging when it is likely to significantly aid in diagnosis and treatment planning.
• MRIs are referred out when patients present with symptoms that suggest serious disc involvement, nerve root compression, or potential surgical indicators. However, MRIs are often not necessary to begin care. A detailed subjective history combined with functional movement and neurological testing is usually sufficient to accurately classify a likely disc injury.
In borderline or unclear cases, we start cautiously, monitor responsiveness, and escalate to imaging only if symptoms persist or fail to improve. When used appropriately, MRI can offer valuable insight, but it should support, not replace, good clinical judgment. [1-4]
However, these static images only tell part of the story. Disc injuries are inherently dynamic, and pain, nerve response, and movement limitations can evolve day to day. What truly guides effective care is how the body is functioning in real time. That’s why we place a strong emphasis on functional assessment: evaluating how the patient stands, moves, compensates, and responds under load. It’s this live, adaptable feedback that drives safe progression and lasting results, especially when a Surbiton Chiropractor is making day-to-day decisions about how quickly to progress your plan.
Red Flags and When to Refer
We understand our scope and respect it. Chiropractic care is not suitable for every disc case.[3][4][7] While non-specialist chiropractors may be able to offer temporary relief by reducing muscular spasm or offloading sensitive tissues, their treatment options are inherently limited. The most important factor is clinical awareness, which involves knowing when to proceed cautiously, when to modify techniques, and when to stop.[3][4][7] Manipulating an inflamed or neurologically reactive disc inappropriately can worsen symptoms.[5][7] Responsible care means recognising when adjustments are contraindicated and prioritising the patient’s long-term outcome over short-term intervention.
However, some cases are above and beyond even good specialist chiropractors like ours; we refer out immediately if there are signs of:
• Cauda equina syndrome (loss of bowel/bladder control)
• Rapid neurological decline
• Fractures, infections, or tumours (require advanced imaging) [3][4]
We collaborate with GPs, orthopaedic consultants, and surgeons when needed to ensure safety and clarity in complex presentations. For someone under the care of a good chiropractor in Surbiton, this joined-up communication is often what gives them confidence that nothing serious is being missed.
What Makes The DISC Protocol Unique?
Our results stem from our knowledge and experience in creating a fully integrated, evidence-led approach that combines technology, structure, and specialist clinical judgment. This is not just a one-size-fits-all method; it’s a specific, structured protocol refined through clinical experience and outcome auditing. The DISC Injury Protocol outlines exactly what to do and when to do it, from decompression timing and laser sequencing to when rehab should begin and which interventions should be avoided early on.[2][3][6][8-16] Each phase is strategically planned to reflect the biology of disc healing, ensuring that every patient progresses through stabilisation, correction, and resilience-building in a sequence proven to deliver consistent results.[1][2][3][6]
People who are searching “Surbiton Chiropractor” or “chiropractor in Surbiton” for a serious disc issue are usually not looking for a quick crack; they are looking for exactly this kind of structured pathway that explains what happens over weeks, not minutes.
• Technology: We utilise spinal decompression to offload injured discs, Class IV laser to calm inflammation and accelerate tissue healing, HIEMT to rapidly restore deep core stability, and radial shockwave therapy to break down chronic adhesions and scar tissue that block progress. [8-20]
• Clinical systems: Our care is driven by functional milestones, not guesswork. Each patient is tracked against objective benchmarks for movement, strength, proprioception, and nerve function across clearly defined phases of care. Reassessments every six visits ensure we stay responsive and targeted.[2][3][6]
• Personalisation: Every plan is customised, but all are grounded in our foundational 18-treatment protocol. This structured framework provides each patient with the necessary exposure to stabilisation, retraining, and resilience-building over 9 weeks. Some patients require more emphasis in the early phases, while others progress quickly into advanced rehabilitation. The key is that we flex within the framework. We adapt based on presentation, reactivity, lifestyle demands, and clinical milestones.[2][3]
• Regenerative: We now live in an era where disc care is no longer limited to managing symptoms or preventing further damage. The focus has shifted to actively influencing the disc’s internal healing environment.
Through decompression, the goal is not only symptom control but also structural improvement. Our protocol is designed to optimise the disc’s ability to rehydrate, reduce internal pressure, and restore mechanical integrity; something that even the best chiropractors in Surbiton are unable to achieve with just their hands, and something surgeons have never even attempted to achieve by cutting parts out.[1][8-11]
Final Thoughts
Having a disc injury can feel overwhelming, but it doesn’t have to be the end of your story. You are not fragile. You are not broken. You may just need the right approach.
If you’ve tried everything else and still feel stuck, this is your sign to take a specialist path forward. Book a discovery call to begin with a comprehensive overview of your symptoms and concerns. You’ll have the opportunity to ask any questions you may have and discuss your medical history, including reviewing your MRI results if you have them. Click here to schedule your free 15-minute spine consult now.
We’ll meet you where you are and help you move again with confidence at The DISC Chiropractors in Surbiton.
References
- Hartvigsen J, Hancock MJ, Kongsted A, et al. What low back pain is and why we need to pay attention. Lancet. 2018;391(10137):2356–2367.
- O’Sullivan PB, Caneiro JP, O’Keeffe M, et al. Unraveling the complexity of low back pain. J Orthop Sports Phys Ther. 2016;46(11):932–937.
- Qaseem A, Wilt TJ, McLean RM, Forciea MA. Noninvasive treatments for acute, subacute, and chronic low back pain: a clinical practice guideline from the American College of Physicians. Ann Intern Med. 2017;166(7):514–530.
- National Institute for Health and Care Excellence (NICE). Low back pain and sciatica in over 16s: assessment and management (NG59). London: NICE; 2016, updated 2020.
- Rubinstein SM, Terwee CB, Assendelft WJJ, de Boer MR, van Tulder MW. Benefits and harms of spinal manipulative therapy for the treatment of chronic low back pain: systematic review and meta analysis. BMJ. 2019;364:l689.
- Goertz CM, Long CR, Vining RD, et al. Effect of usual medical care plus chiropractic care vs usual medical care alone on low back pain and disability in active duty military personnel: a randomized clinical trial. JAMA Netw Open. 2018;1(1):e180105.
- Gorrell LM, Engel RM, Brown B, et al. Reporting of adverse events associated with spinal manipulation: a systematic review. Musculoskelet Sci Pract. 2023;64:102704.
- Macario A, Richmond C, Auster M, Pergolizzi J. Spinal decompression via motorized traction for chronic discogenic low back pain: a systematic literature review. Pain Pract. 2008;8(1):11–17.
- Daniel DM. Nonsurgical spinal decompression therapy: a systematic review of the literature. J Chiropr Med. 2007;6(3):139–145.
- Amjad F, Bukhari SR, Malik AN, et al. Effects of nonsurgical spinal decompression therapy in addition to core stabilization exercises on chronic low back pain. BMC Musculoskelet Disord. 2022;23(1):1013.
- Choi E, Choi KH, Hwangbo G. Effect of nonsurgical spinal decompression therapy on pain and lumbar functional disability in patients with lumbar disc herniation. J Back Musculoskelet Rehabil. 2022;35(1):53–59.
- Abdildin Y, Abylkassov R, et al. High intensity laser therapy in low back pain management: a systematic review and meta analysis. Lasers Med Sci. 2023;38(5):1–15.
- Alayat MSM, Alshehri MA, Aly THA. Long term effect of high intensity laser therapy in the treatment of patients with chronic low back pain: a randomized blinded placebo-controlled trial. Lasers Med Sci. 2014;29(3):1065–1073.
- Abdelbasset WK, Nambi G, Elsayed SH, et al. A randomized comparative study between high intensity and low level laser therapy in chronic non specific low back pain. J Lasers Med Sci. 2020;11(2):200–205.
- Huang Y, Wang Y, et al. The effectiveness of high intensity laser therapy for low back pain: a randomized controlled trial. Medicine (Baltimore). 2020;99(39):e22200.
- Mulyadi A, et al. Comparing the effectiveness of high and low intensity laser therapy in enhancing conventional treatment for musculoskeletal pain: a systematic review. 2025.
- Yue L, Zhang Z, et al. Extracorporeal shockwave therapy for treating chronic low back pain: a systematic review and meta analysis of randomized controlled trials. Biomed Res Int. 2021;2021:1–11.
- Liu K, Zhang S, et al. Efficacy and safety of extracorporeal shockwave therapy in chronic low back pain: a systematic review and meta analysis. J Orthop Surg Res. 2023;18(1):139.
- Wu Z, Huang H, et al. Extracorporeal shockwave therapy for low back pain: a meta analysis. Medicine (Baltimore). 2023;102(17):e33110.
- Ferdinandov D, et al. Focused extracorporeal shockwave therapy for chronic low back pain: a systematic review and meta analysis. Front Med. 2024;11:1376542.
- Weber H. Spine Update: The Natural History of Disc Herniation and the Influence of Intervention. Spine 1994; 19:2234-8.
- Cassidy J, Thiel H and Kirkaldy-Willis W. Side Posture manipulation for Lumbar Intervertebral Disk Herniation. Journal of Manipulative and Physiological Therapeutics 1993; 16(2):96-103.
- Slosberg M. Side Posture Manipulation for Lumbar Intervertebral Disk Herniation Reconsidered. Journal of Manipulative and Physiological Therapeutics 1994; 17(4):258-62.
- Crawford, R., J. & al., e. (1994). Back pain in primary care. Outcomes at 1 year. Journal of Clinical Epidemiology 47. https://pubmed.ncbi.nlm.nih.gov/8316884/
- (2025). Diagnostic Imaging Practice Guidelines for Musculoskeletal Complaints in Adults. National Imaging Associates, Inc. Diagnostic Imaging Practice Guidelines for Musculoskeletal Complaints in Adults. https://cms.radmd.com/sites/default/files/2023-09/2023-nia-physical-medicine-guidelines.pdf